Roadmap
Improving Out-of-Hospital Cardiac Arrest Survival
A Roadmap For Achieving Resuscitation Excellence

Step 1 — Measure to Improve
The Chain of Survival looks uniquely different in every community. The variability may be due to design. Often, links have missing or broken pieces that translate to sub-optimal conditions to save a live.
Improving cardiac arrest survival is a process. With so many moving parts, its can be difficult to know where to begin improvements.
Measuring gaps in the Chain of Survival provides clarity on where to focus. Once gaps are understood, focused programs may improve performance. Sometimes there is a process defect that affects speed and quality. Other times delayed provision of care or provider’s skill decay can lead to unexpected outcomes.
We believe every community should measure its Chain of Survival and commit to a plan of continuous improvement.
Step 2 – Close Performance Gaps?
Does the quality of EMS provider’s education have an impact on cardiac arrest survival? Yes.
Traditional resuscitation training programs lack many of the essential instructional design features necessary to improve learning. When training is insufficient, and measurement of learning outcomes are absent, harm may occur to patients.
Clinical and educational experts researched the literature for evidence about what leads to effective performance during resuscitations. Their findings are published in the AHA Scientific Statement on Resuscitation Education Science.
Providers learn and retain critical resuscitation skills when the Resuscitation Education concepts are applied. RQI Programs are designed using these evidence-based methods.

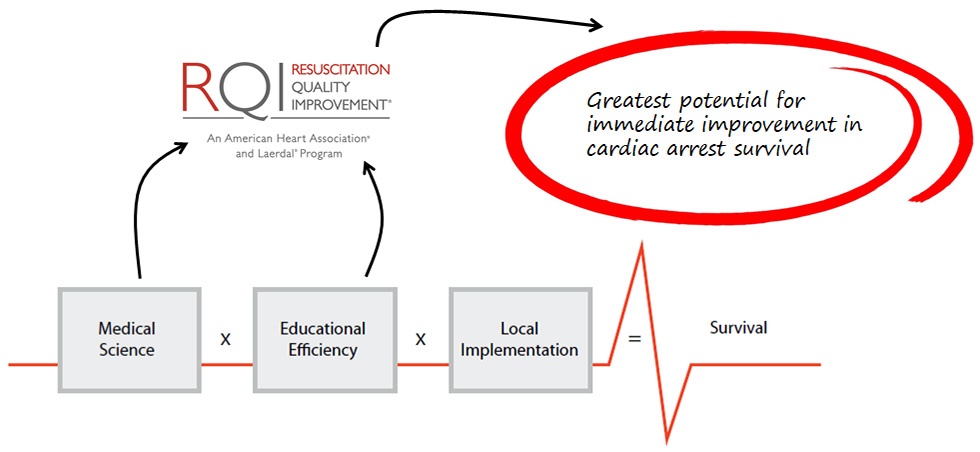
Step 3 – Implement and Continuously Improve
Quality improvement is a process, not an event. The potential to improve cardiac arrest survival is enormous. However, the potential rests within a short window of time – just 600 seconds from the start of an incident until potentially irreversible brain death. To increase survival, communities should focus on a whole system of care approach with emphasis on local implementation and continuous improvement.
Continuous clinical improvement requires sustained and focused effort. We recognize measurement and analysis is time-consuming. Spaced learning and tailored feedback is difficult to achieve with limited resources. That’s why RQI Partners developed a programmatic approach to continuous improvement.